Last updated on
Patients Are Asking: What’s The Link Between Blood Clots and Cancer?

Dr. Jean Connors is the Medical Director of the Anticoagulation Management Service at Brigham and Women’s Hospital and Dana-Farber Cancer Institute. Dr. Connors provides some insights.
Q: Blood clots are a known complication in cancer patients— but how common are they?
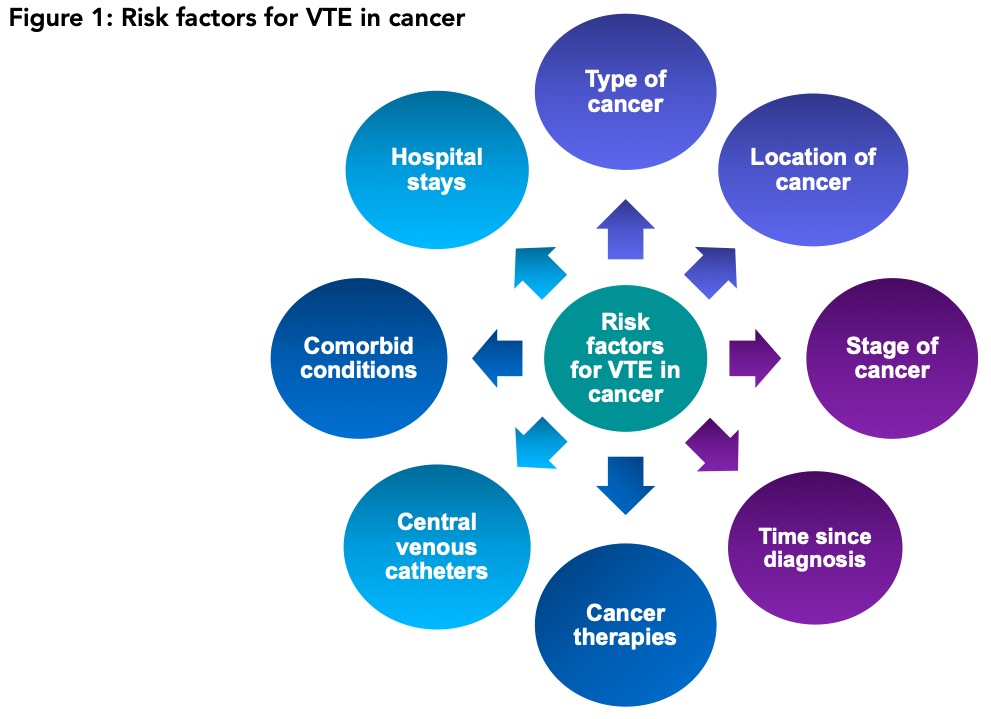
If you consider everyone with a blood clot today, roughly 20% of those people have cancer. Cancer is a very strong risk factor for developing a clot. Certain types of cancers are more associated with clots, such as pancreatic and stomach cancer. Some chemotherapy and radiation treatments also increase the risk of blood clots, along with several other factors (Figure 1).
Q: Why are some cancers more likely to lead to a blood clot than others?
Certain cancers can release substances from the cells that activate coagulation, thereby forming a clot. Sometimes, a mass—or lymph nodes—will compress the blood vessels and slow blood flow, which also results in a clot.
Q: Are there any preventative measures that a person can take once they find out they are diagnosed with cancer?
Patients should remain active if they can and should talk to their providers about whether preventive anticoagulation would benefit them based on their individual risk factors. Two of the direct oral anticoagulants (DOACs) have been studied in this area—rivaroxaban (Xarelto®) and apixaban (Eliquis®) both work well at preventing blood clots with minimal bleeding.
Q: What’s the current treatment protocol for clots in cancer patients?
Low-molecular-weight heparin (LMWH) injections used to be the gold standard, but now it’s acceptable to use a DOAC. We’ll still use LMWH if we’re concerned about gastrointestinal (GI) tract bleeding, nausea and vomiting from chemotherapy, or other factors.
Q: Should patients expect their oncologist to help them manage a clot?
I think it depends on the comfort level of the patient and the medical oncologist, as well as the complexity of the blood clot and the treatment. In many situations, patients would benefit from seeing a blood clot specialist in vascular medicine, cardiology, or hematology.
*Originally published in The Beat – October 2019. Read the full newsletter here.